Stem cell therapy—particularly treatments based on mesenchymal stem cells (MSCs)—is one of the most promising frontiers in regenerative medicine today. These therapies harness the body’s own healing potential to support tissue repair, reduce chronic inflammation, and restore function in areas damaged by injury or disease.
Patients across the U.S. and around the world are seeking stem cell treatments for a variety of conditions, including osteoarthritis, autoimmune diseases like rheumatoid arthritis or multiple sclerosis, degenerative spinal issues, and sports-related injuries. But understandably, many ask the same core question before beginning their regenerative journey:
“What are the real success rates of stem cell therapy?”
In this section, we break down current evidence from both clinical studies and real-world patient outcomes, explaining what success means, how it is measured, and what factors can influence your results. Whether you’re considering stem cell therapy for pain, mobility, inflammation, or recovery, this guide will help you make a confident and informed decision.
How Do We Measure Success in Stem Cell Treatments?
Not every patient is looking for the same outcome—and not all success looks the same. In personalized regenerative medicine, success is defined by improvements that align with each person’s health goals and baseline condition.
We typically look at the following measurable indicators to define success:
- Pain Reduction: A significant decrease in chronic or acute pain, especially in joints, spine, or soft tissues.
- Improved Function & Mobility: Better range of motion, balance, strength, or coordination—particularly in orthopedic and neurological cases.
- Lower Dependence on Medication: Many patients reduce or stop using painkillers, anti-inflammatories, or immunosuppressants after treatment.
- Improved Energy & Vitality: Fatigue and brain fog often improve, particularly in patients with systemic inflammation or post-viral syndromes.
- Objective Improvements: MRI results, X-rays, or lab markers (e.g., reduced inflammatory cytokines) that show tissue repair or slowed degeneration.
Success is not always instant—but with the right patient profile, the right protocol, and proper follow-up, results are both measurable and meaningful.

Success Rates by Condition: Clinical Outcomes Backed by Experience & Research
| Condition Treated | Reported Success Rate* |
| Knee Osteoarthritis | 75–85% improvement |
| Autoimmune Conditions (RA, MS) | 65–75% symptom relief |
| Spinal Disc Degeneration | 60–70% pain reduction |
| Sports Injuries | 80–90% recovery support |
| Long COVID / Chronic Fatigue | 50–65% improvement |
*Data based on peer-reviewed publications, outcome surveys, and in-clinic follow-ups.
It’s important to note that MSC therapy doesn’t “cure” disease—but it often helps modulate the immune system, regenerate soft tissues, and delay or reduce the need for surgery.

Ready to get started?
Fill out a brief patient screening application and find out if you are a candidate for our stem cells therapies.
What Affects Stem Cell Success?
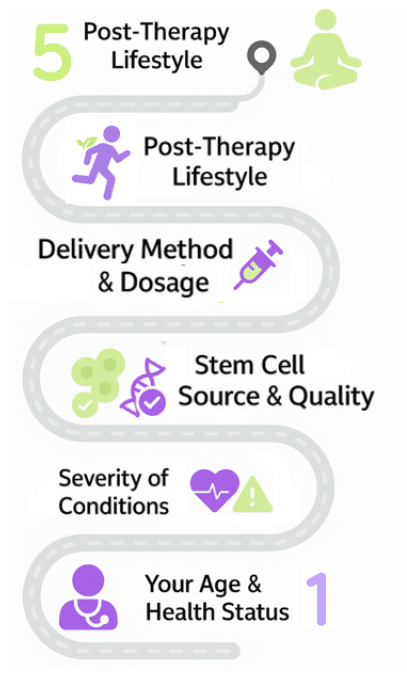
Just like any therapy, stem cell outcomes depend on biological and procedural variables. At our clinic, we consider these top five factors when determining your potential for success:
- Your Age & Health Status: Younger patients or those with less systemic inflammation tend to heal faster. However, older adults still benefit, especially with proper nutrition and immune support.
- Severity of the Condition: Early-to-moderate stage diseases respond better. If tissue damage is advanced, results may be limited but still meaningful.
- Stem Cell Source & Quality: We use Cellureon products, with high-purity and clinically processed MSCs and its derivatives (COLOCAR ENLACE).
- Delivery Method & Dosage: Proper cell count, injection technique, and support therapies (see our Cellular Optimization Protocol) greatly influence effectiveness.
- Post-Therapy Lifestyle: Anti-inflammatory diets, physical therapy, and sleep support can help maximize your body’s regenerative response.